Allergic reactions are common, but severe ones are not. They require quick action. Every second is critical.
Anaphylaxis is a severe allergic reaction. It can make breathing hard and lower blood pressure. It’s a medical emergency that needs immediate treatment.
You can learn to spot and handle severe allergic emergencies. Knowing how can save lives. It could be a family member, friend, or even a stranger.
This guide will teach you the necessary skills. You’ll learn to recognize severe reactions and use epinephrine. You’ll also know what to do after giving the medicine.
Being prepared is easy with the right knowledge. Let’s start your journey to help in emergencies.
Table of Contents
Understanding Severe Allergy First Aid and Anaphylaxis
Allergic reactions can be mild or very serious. Some might just cause a little discomfort. But others need emergency care right away. It’s important to know the difference to get the right help fast.
Not all allergic reactions are the same. The severity depends on how many parts of your body are affected and how fast symptoms show up. When your immune system reacts too strongly, it releases chemicals that cause different reactions. The severity depends on the allergen, your sensitivity, and how your body reacts.
What Makes an Allergic Reaction Severe
A severe allergic reaction affects more than one part of your body. You might have trouble breathing and also have skin reactions or stomach issues. Swelling in your face and neck is another sign.
Severe reactions include:
- Difficulty breathing or wheezing
- Swelling of the face, neck, tongue, or lips
- Rapid or weak pulse
- Dizziness or confusion
- Severe drop in blood pressure
- Loss of consciousness
If your breathing or heart is affected, you need help fast. These signs mean you need life-threatening allergy care right away.
The Difference Between Mild Reactions and Life-Threatening Anaphylaxis
Mild reactions usually stay in one area and develop slowly. You might get itching in your mouth, a small rash, or a stuffy nose. These can be treated with over-the-counter antihistamines and don’t spread.
| Mild Allergic Reactions | Life-Threatening Anaphylaxis |
|---|---|
| Red, watery eyes | Swelling of airways restricting breathing |
| Localized hives or skin rash | Swelling of face, neck, throat, and tongue |
| Stuffy or runny nose | Difficulty breathing or gasping for air |
| Mild itching or discomfort | Rapid, weak, or irregular heartbeat |
| Abdominal cramps or nausea | Dizziness, confusion, or loss of consciousness |
| Treatment: Antihistamines sufficient | Treatment: Epinephrine auto-injector required immediately |
Anaphylaxis is life-threatening and can happen fast, sometimes in minutes. Your airways swell, making it hard to breathe. Your heart rate goes up, blood pressure drops, and you might feel dizzy or confused. This is when you need life-threatening allergy care, with immediate epinephrine injection and emergency services.
The key is: if symptoms show up in more than one area at once, it could be severe. If you’re unsure, call emergency services right away. Epinephrine auto-injectors are for severe reactions, not mild allergies.
Recognizing the Warning Signs of a Severe Allergic Emergency
Speed is key in a severe allergic emergency. Spotting warning signs early helps you act fast. Anaphylaxis can happen quickly, sometimes in just minutes. Knowing the signs can save a life. It’s all about understanding the acute allergic emergency protocol.
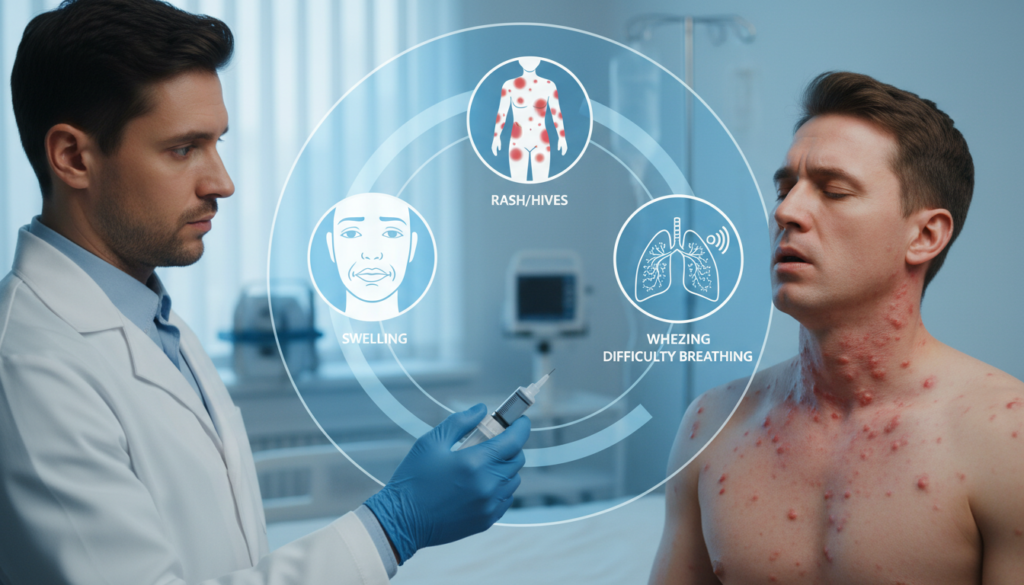
Severe allergic reactions show up in different ways. First, watch for respiratory symptoms. Look for wheezing, trouble breathing, throat tightness, and a hoarse voice. These signs mean your airway is narrowing.
Next, notice cardiovascular warnings. A rapid or weak pulse, dizziness, fainting, or pale skin are signs of trouble. These symptoms mean your body isn’t getting enough oxygen-rich blood. This is when anaphylactic shock procedures become critical.
Swelling is also important. Look for sudden puffiness in the face, lips, tongue, or throat. Widespread hives or a raised, itchy rash across the skin are red flags. Your skin might appear flushed or very pale.
Stomach problems can also appear. Severe belly pain, nausea, vomiting, or diarrhea may develop. Some people feel confused, drowsy, or unusually thirsty.
| Body System | Warning Signs to Watch |
|---|---|
| Breathing | Wheezing, rapid breathing, throat tightness, trouble swallowing |
| Heart and Blood | Weak or rapid pulse, dizziness, fainting, pale skin |
| Skin | Swelling of face or throat, widespread hives, rash |
| Stomach | Severe pain, nausea, vomiting, diarrhea |
Understanding anaphylactic shock procedures means recognizing that shock is a life-threatening condition. When shock develops, your body’s organs don’t receive enough oxygen. Without quick treatment, systems begin to fail. This is why the acute allergic emergency protocol emphasizes acting within minutes.
- Act fast when you spot any of these signs
- Trust your instinct if something feels seriously wrong
- Call 911 immediately—don’t wait to see if symptoms improve
- Use an epinephrine auto-injector if available
Recognizing these warning signs early gives you the power to respond quickly and effectively. Your knowledge and quick action can mean the difference between a bad scare and a tragedy.
Administering Epinephrine: The Critical First Response
When someone shows signs of anaphylaxis, epinephrine is the only medication that can save their life. This powerful drug works fast to reverse the dangerous symptoms by constricting blood vessels, increasing heart rate, and opening airways. Knowing how to use epinephrine auto-injector devices properly can mean the difference between life and death. This section walks you through the exact steps and timing needed to act with confidence during a medical emergency.
How to Use an Epinephrine Auto-Injector Properly
Epinephrine auto-injectors come pre-filled with a single dose of medication. Learning proper EpiPen administration steps ensures you can act quickly and correctly when minutes count.
Follow these steps for correct epinephrine auto-injector use:
- Remove the auto-injector from its carrier tube
- Hold the device firmly with the orange tip pointing downward
- Remove the blue safety cap by twisting it off
- Place the orange tip against the outer thigh, even through clothing
- Push down firmly until you hear a distinct click sound
- Hold the injector in place for about 3 seconds
- Remove the injector and massage the injection area for 10 seconds
The person should sit or lie down in a comfortable position while waiting for emergency services. Never put your thumb or fingers on the orange tip during injection.
| Step | Action | Important Detail |
|---|---|---|
| 1 | Remove from carrier | Handle with care and confidence |
| 2 | Hold firmly, orange tip down | Orange tip must point downward |
| 3 | Remove blue safety cap | Twist cap to remove it |
| 4 | Apply to outer thigh | Works through clothing |
| 5 | Push down until click | Full force may be needed |
| 6 | Hold for 3 seconds | Count slowly to ensure full delivery |
| 7 | Remove and massage | Massage for 10 seconds after removal |
When to Administer the Medication and Call 911
Give epinephrine immediately if someone shows signs of anaphylaxis. Do not wait to see if symptoms improve on their own. It’s always better to use it and not need it than to delay and risk serious harm or death.
If you’re alone with the person experiencing anaphylaxis, follow this order:
- First, assist with administering the epinephrine auto-injector
- Then call 911 right away
- Stay with the person until help arrives
Calling emergency services is not optional after giving epinephrine. Symptoms can return or get worse within minutes. Paramedics need to provide professional care and monitor the person’s condition closely.
Always carry two auto-injectors if you have severe allergies. A second dose may be needed if symptoms don’t improve within 5 to 15 minutes. Never substitute antihistamines for epinephrine during a serious allergic reaction. Antihistamines work too slowly and cannot reverse anaphylaxis. Epinephrine is the only treatment that stops this life-threatening emergency.
Common Triggers and Prevention Strategies for Anaphylactic Reactions
Understanding what causes severe allergic reactions is key to a good emergency plan. Many things can trigger anaphylaxis, from foods to insect stings to medicines. Knowing these triggers helps keep you safe and ready for emergencies.
Foods are the main cause of severe reactions. The “Big Eight” allergens include peanuts, tree nuts, shellfish, milk, eggs, soy, wheat, and fish. Even small amounts can be deadly for those who are allergic. Insect venom from bees, wasps, hornets, yellow jackets, and fire ants also poses serious risks for people with sting allergies.
Medicines like penicillin and sulfa drugs can cause dangerous reactions in some patients. Latex, found in medical gloves and balloons, triggers anaphylaxis in latex-sensitive people. Environmental allergens such as certain pollens and animal dander rarely cause anaphylaxis but can affect some individuals severely.
Prevention Strategies for Your Emergency Allergy Response
Creating a strong prevention plan requires awareness and preparation. Start by reading food labels carefully and telling restaurants and food preparers about your allergies. Wearing a medical alert bracelet or necklace tells emergency responders about your condition immediately.
- Keep two epinephrine auto-injectors with you at all times
- Educate family members and coworkers about your allergies
- Develop allergy action plans for schools and workplaces
- Avoid latex products if you have latex sensitivity
- Stay indoors during peak insect season if needed
- Create allergen-free zones in your home
The “rule of two” is critical for your emergency allergy response preparedness. Always carry a backup epinephrine device in case the first one malfunctions or you need a second dose. Store one injector with you and keep another in an easy-to-access location at home, school, or work. Complete avoidance of allergens isn’t always possible, so combining vigilance with proper medication access creates the strongest protection against severe reactions.
Conclusion
You now know how to handle severe allergic reactions confidently. Severe Allergy First Aid means knowing the difference between mild and life-threatening reactions. You learned to spot warning signs quickly.
You also learned how to use an epinephrine auto-injector correctly. Understanding common triggers and prevention strategies is key. This knowledge is important for everyone, not just those with allergies. You could save a life someday.
If you have severe allergies, take action now. Make sure you have the latest prescriptions for epinephrine auto-injectors. Carry two auto-injectors with you always and check their expiration dates.
Show your family and friends where you keep them. Teach them how to use them. Wear medical alert jewelry to alert others about your allergy. Visit resources about anaphylaxis to stay safe. Talk to an allergy specialist for more advice.
Are you a family member, friend, teacher, or coworker of someone with severe allergies? Ask to see their emergency action plan. Learn how their auto-injector works. Know the warning signs to watch for.
Consider taking a first aid class that covers anaphylaxis response. Your knowledge can make a big difference. Severe Allergy First Aid training gives you confidence.
Being prepared removes fear and gives you power. Knowledge and practice are your best tools. By reading this guide, you’ve taken a big step toward responding in an allergic emergency. Stay ready, stay informed, and remember: you have what it takes to help.
FAQ
What’s the difference between a mild allergic reaction and a severe allergic emergency?
A mild allergic reaction might cause hives, itchy skin, or a stuffy nose. But it doesn’t stop you from breathing or acting normally. On the other hand, a severe reaction affects many parts of your body at once. It can make breathing hard, cause swelling, or make your heart race.
Life-threatening anaphylaxis is the worst kind. It happens when your body can’t get enough oxygen. This can lead to anaphylactic shock if not treated right away. Severe reactions get worse fast and can be deadly in minutes.
What are the early warning signs that someone is experiencing anaphylaxis?
Spotting anaphylaxis early is key. Look for signs like wheezing, trouble breathing, or throat tightness. Also, watch for a fast or weak pulse, dizziness, or a sudden drop in blood pressure.
Signs of swelling, widespread hives, or pale skin are also important. Gastro issues like severe pain, nausea, or diarrhea are other red flags. If someone’s heartbeat is too fast, they’re breathing too quickly, or their skin looks pale, it’s a sign of anaphylactic shock.
How do I properly use an epinephrine auto-injector like an EpiPen?
Using an EpiPen is straightforward but critical. First, take it out of its carrier tube. Hold it with the orange tip down and remove the blue safety cap.
Place the orange tip on the thigh, and push down until you hear a click. Hold for 3 seconds to ensure the full dose is delivered. Remove the injector and massage the area for 10 seconds to help absorption.
Should I call 911 before or after administering epinephrine?
Give epinephrine first if someone’s having a severe reaction. Then, call 911 right away. If you’re alone, use the epinephrine and then call for help.
Remember, epinephrine buys you time while you wait for medical help. Even after using it, call for emergency services. They need to monitor you for complications and may give more doses.
What are the most common triggers for severe allergic reactions and anaphylaxis?
Common triggers include food allergens like peanuts, tree nuts, shellfish, and milk. Insect venom and certain medications also cause severe reactions. Latex and environmental allergens like pollen can trigger reactions too.
Knowing your triggers is key to preventing severe reactions. Always carry two epinephrine auto-injectors, as you might need a second dose.
How can I prevent severe allergic reactions in my daily life?
Prevention involves being vigilant and prepared. Read labels carefully and inform restaurants about your allergies. Wear a medical alert bracelet or necklace.
Teach family, friends, and coworkers about your allergies. Create an allergy action plan for schools and workplaces. Always carry two epinephrine auto-injectors.
What should I do if I witness someone having a severe allergic reaction but don’t have their epinephrine auto-injector?
Call 911 immediately and give them details about the person’s symptoms. Keep the person lying down with legs elevated unless they’re having trouble breathing.
Monitor their breathing and consciousness. If they have an auto-injector, ask them to use it. Don’t give them food or water. Reassure them help is on the way.
Can antihistamines treat anaphylaxis, or do I always need epinephrine?
Antihistamines should never replace epinephrine for anaphylaxis. They work too slowly for severe reactions. Epinephrine is the only fast-acting treatment for anaphylaxis.
Use epinephrine immediately if someone is having a severe reaction. Antihistamines may be used later, but they’re not a substitute for epinephrine.
How quickly can anaphylaxis develop, and why is immediate action so important?
Anaphylaxis can happen in minutes, sometimes faster. It’s a severe reaction that can quickly become life-threatening. Without quick action, it can lead to shock.
Recognizing early signs and acting fast is critical. Even if unsure, it’s better to use epinephrine than to wait and risk death.
What medical alert identification should someone with severe allergies wear?
Someone with severe allergies should wear a medical alert bracelet or necklace. It should clearly state their allergies and that they carry an epinephrine auto-injector. This identification is vital for emergency responders.
Keep a wallet card with the same information as backup. Inform people close to you about the importance of this identification.
How often should someone with severe allergies check and replace their epinephrine auto-injectors?
Check epinephrine auto-injectors monthly. Mark your calendar to remember. Expired medication may not work in emergencies.
Replace auto-injectors by their expiration date or after use. Insurance often covers two per prescription. Store them at room temperature and keep them accessible.
Should I inform my employer and coworkers about my severe allergies?
Yes, absolutely. Informing your employer and coworkers about your allergies is important. Provide them with your allergy action plan and identify a coworker who can help in an emergency.
Let them know about your specific triggers. Request a safe place to store your epinephrine auto-injectors. Some workplaces may keep extra auto-injectors on hand.
What’s the difference between an allergic reaction and anaphylactic shock?
An allergic reaction is your body’s response to a perceived threat. It can range from mild to severe. Anaphylaxis is a severe reaction that affects many body systems and can be life-threatening.
Anaphylactic shock is the most severe stage of anaphylaxis. It happens when your body can’t get enough oxygen. Symptoms include a fast heartbeat, rapid breathing, and pale skin.
Can someone have anaphylaxis without a prior allergic reaction to the same substance?
Yes, absolutely. Anaphylaxis can happen on the first exposure to an allergen. It’s a severe immune response that doesn’t require a history of milder reactions.
Some people’s immune systems are more prone to severe reactions. Cross-reactivity can also occur, where exposure to one substance triggers reactions to similar substances. Be aware of your body’s reactions and seek testing if you suspect severe allergies.
Is it safe to use an epinephrine auto-injector if I’m not completely sure someone is having anaphylaxis?
Yes, it’s safe to use epinephrine when unsure. Medical experts agree it’s better to use it and not need it than to delay and risk death. Epinephrine has been used safely for decades.
If someone is showing signs of anaphylaxis, give them epinephrine right away. Call 911 after administering it. Let medical professionals decide if anaphylaxis occurred and provide further treatment.
What should I do if someone refuses to let me give them their epinephrine auto-injector during what appears to be anaphylaxis?
If someone refuses epinephrine during anaphylaxis, it’s a tough situation. Explain that it’s necessary to save their life. If they’re having trouble breathing or seem confused, prioritize their safety.
Call 911 and describe the situation. Encourage the person to accept the medication while keeping them calm. If their condition worsens, you may need to act quickly to save their life.
How can I educate my child’s school about their severe allergies and ensure they’re prepared?
Create a detailed allergy action plan with the school, healthcare provider, and school nurse. Include a list of your child’s allergens and how to recognize anaphylaxis symptoms.
Teach the school how to use your child’s epinephrine auto-injector. Make sure they know what to do in an emergency. This preparation helps keep your child safe at school.